Childhood leishmaniasis: Report of 106 cases
Published Web Location
https://doi.org/10.5070/D30x40s44gMain Content
Childhood leishmaniasis: Report of 106 cases
Monia Kharfi MD1, Rym Benmously MD2, Nadia El Fekih MD1, Meriem Daoud MD1, Zohra Fitouri MD3, Inçaf Mokhtar2, Saïda Ben Becher MD3, and Mohamed Ridha Kamoun MD1
Dermatology Online Journal 10 (2): 6
From the Dermatology Department, Charles Nicolle Hospital1, Dermatology Department, Habib Thameur Hospital 2, and Pediatric Department, Childrens Hospital3, Tunis, Tunisia. monia.kharfi@rns.tn
Abstract
In Tunisia there are three epidemic clinical forms of cutaneous leishmaniasis. They are associated with three different species of Leishmania and are observed in different geographical areas. We undertook a single-center retrospective analysis of childhood leishmaniasis in order to describe epidemio-clinical profile, therapeutic characteristics and clinical outcomes of affected patients. The study comprises 166 children with 132 lesions of cutaneous leishmaniasis. The subjects ages range from 5 months to 15 years (average 8.75 years). The F:M sex ratio is 1.3. Leishmaniasis affects grown-up children in 74.5 percent of the cases. All of our patients live in an endemic area. The face is affected in 76.5 percent of cases. Mucosal leishmaniasis is present in 9 children (6.8 %). Clinical diagnosisis confirmed by the parasitologic smear or hispathological examination in 89.6 percent of the cases. Treatment with intralesional meglumine antimoniate is done for 67 patients; the treatment regimen is one local injection (1 ml/cm²) per week until recovery. Systemic meglumine antimoniate is the initial therapy for 25 patients. Meglumine antimoniate treatment is well tolerated with no side-effects. All leishmaniasis lesions heal within an average period of 2.18 months. Childhood cutaneous leishmaniais is common in Tunisia. It has the characteristics of sporadic leishmaniasis. Mucosal leishmaniasis has a favorable outcome with no destruction, nor scaring defomity. The standard treatment remains intralesional meglumine antimoniate.
Background
Leishmaniasis is a protozoan disease that is transmitted by the sandfly. It occurs widely throughout Africa, Asia, South America, the Middle East, and the Mediterranean region. In Tunisia three epidemic clinical forms are recognized. They are associated with three different species of Leishmania and are observed in different geographical area.
Cutaneous leishmaniasis affects both adults and children. Through the analysis of a monocentric study concerned with childhood leishmaniasis, we aim to describe the epidemio-clinical profile, therapeutic characteristics, and outcome data of this dermatosis.
Patients and methods
We conduct a retrospective study covering an 11-year period (1989-2000) in the dermatology department of Charles Nicolle hospital in Tunisia. All medical reports of cutaneous leishmaniasis are reviewed. Patients included are younger than age 16.
The diagnosis of cutaneous leishmaniasis is based on a clinical presentation, a positive parasitic smear, or a contributive histopathology. Information is gathered for each patient, including age, sex, geographic location, previous history of leishmaniasis, a stay in an endemic area, the month of consultation, lesion location, and the number and size of lesions. Laboratory investigations include a blood chemistry analysis in cases of systemic drug administration. We also note treatment and outcome.
Results
During this 11-year period, information on 106 children with 132 lesions of cutaneous leishmaniasis was collected. Childhood cutaneous leishmaniasis represented 30.2 percent of all cutaneous leishmaniasis cases in our dermatology department during that period. Affected children had an average age of 8.75 years. The youngest patient was 5 months old and the oldest was age 15. Distribution according to age showed that leishmaniasis affected older children (6-15 years) in 74.5 percent of the cases. The sex ratio (F 61:M 45) was of 1.3. All of our patients lived in an endemic area. The majority of the patients come from northern parts of the country (82.5 %) followed by the center (11.3 %) and the south (6.6 %). The patients gave a history of cutaneous leishmaniasis in other family members in 5.6 percent of the cases.
|
|
| Figure 1 | Figure 2 |
|---|---|
|
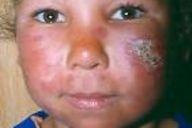
Papulosquamous, erythematous, infiltrated lesions of the face (Fig. 1). |
|
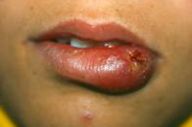
| Nodular, crusted lesion of the labial mucosa (Fig. 2). | |
|
|
| Figure 3 | Figure 4 |
|---|---|
|
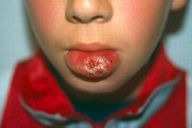
Giant nodule with eversion of the lower lip (Fig. 3). |
|
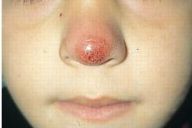
| Erythematous, nodular lesion of the tip of the nose (Fig. 4). | |
The face was the most commonly affected site (76.5 %). The cheek was the site of involvement in 40.5 percent (Table I). The duration of disease at the time of presentation ranged from 20 days to 5.5 years with an average duration of 8 months. Mucosal leishmaniasis was present in 9 children (6.8 %). Lesions affected the labial corner (4 children), the lips (3 children), and the nose (2 children).
| Location | Number | (%) |
|
|
||
| Cheek | 53 | (40.5) |
| Cace front | 15 | (11.4) |
| Nose | 7 | (5.3) |
| chin | 4 | (3.1) |
| Periocular | 3 | (2.3) |
| Mucosal | 9 | (6.8) |
| Upper limb | 18 | (13.6) |
| Lower limb | 9 | (6.8) |
|
|
||
|
|
| Figure 5 | Figure 6 |
|---|---|
|
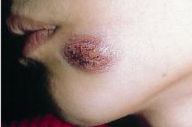
Lupoid plaque of the cheek (Fig. 5). |
|
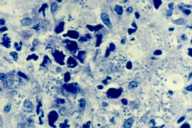
| Giemsa stain of the dermal infiltrate revealing pale blue amastigotes (Fig. 6). | |
We encountered four clinical forms of leishmanias: papulo-nodular (76.2 %), mucocutaneous (6.8 %), lupoid (12 %) (Fig. 5), and furonculoid (1.5 %). Clinical diagnosis was confirmed by the parasitologic smear or by the hispathological examination in 89.6 percent of the cases. In five cases (4.7 %) the histopathologic examination revealed the diagnosis showing a dermal infiltrate of lymphocytes, plasma cells, and macrophages filled with leishmania organisms. Giemsa stain revealed amastigotes, which appear pale blue (Fig. 6). In the remaining six patients, a suggestive clinical presentation associated with a history of a travel to an endemic area (five patients) or a family history of leishmanisis (one case) were used to make the diagnosis. Treatment was well documented in 100 patients (94.3 %). Five patients were lost to followup and one child healed spontaneously.
Sixty-seven patients (63.2 %) underwent treatment with intralesional meglumine antimoniate, given as one injection (1 ml/cm²) per week until recovery (10 days-1 year). The average number of injections was about 1.9. Systemic meglumine antimoniate therapy (60 mg/kg/day for 7-15 days) was initially prescribed for 25 patients. Meglumine antimoniate treatment was well tolerated without side-effects. Cryotherapy was used in one patient as an adjunct to intralesional meglumine antimoniate and in another patient for a lupoid lesion of the cheek. Surgical removal of a tumor of the nasal mucosa revealed leishmaniasis on histology. In one girl, the combination of metronidazole and pentamidine was pescribed because of resistance to multiple courses of meglumine antimoniate.
Follow-up records were available for 57 patients. All leishmaniasis lesions healed within an average period of 2.18 months. Hyperpigmented scars were seen in 26.3 percent of the patients, milium grains in 7.01 percent, atrophic scars in 3.5 percent, and hypopigmented scars in 3.5 percent. Complete recovery without scars occurred in 59.6 percent.
Discussion
Leishmaniasis is quite prevalent in Tunisia. The distribution is both in endemic areas and sporadic throughout the country [1, 2, 3, 4]. The arthropod vector for all forms of leishmaniasis is the female sandfly. Adult female sandflies require a blood meal. During blood feeding, infected sandflies inject saliva containing leishmania organisms into the wound. The transmission cycle of the leishmania organisms requires an arthropod vector and a mammalian reservoir. In the insect vector, the parasites are flagellated and extracellular; the organism is in its flagellated, promastigote form. Once inside the human, canine, or rodent host, the parasites are internalized by dermal macrophages. Here, they exist as intracellular, nonflagellated amatigotes. The cycle is completed when the sandfly feeds on an infected host, and the parasite moves to the gut where metamorphosis into the promastigote form takes place.
The various disease expressions are associated with several different organisms of the genus leishmania. Three epidemic clinical forms have been distinguished since 1988. Sporadic cutaneous leishmaniasis found in northern Tunisia is caused by Leishmania infantum. Zoonotic cutaneous leishmaniasis is epidemic in central and southern Tunisia and is caused by Leishmania major. Anthroponotic cutaneous leishmaniasis is endemic in southeastern Tunisia and is caused by Leishmania tropica [1]. Some previous studies found that the distribution of childhood cutaneous leishmaniasis is similar to that of childhood kala-azar [5, 6, 7].
In our study, childhood leishmaniasis is frequent and affects mostly school-age children with a history of stay in an endemic area. Even infants can be affected. Most of our patients originate from the northern parts of the country (82.1 %), which may be associated with the geographical situation of our hospital. A family history of leishmaniasis is relatively frequent (5.6 %), and it is necessary to examine all family members. There is no visceral leishmaniasis, nor post-kala-azar leishmaniasis in this area. The delay for consultation is relatively long (8 months), attesting to the insidious and mild character of cutaneous leishmaniasis. As in adults, morphological findings are those of sporadic leishmaniasis [1, 2]. Lesions occur mostly on the face and are unique and small. There are no seasonal outbreaks.
Although South American mucocutaneous leishmaniasis caused by Leishmania braziliensis results in mutilating and disfiguring lesions [8, 9], Tunisian mucosal leishmanisis caused by dermotropic Leishmania major has a favorable outcome with no mutilations [3, 10, 11, 12].
Cutaneous leishmaniasis lesions can be misdiagnosed, especially in children, with impetigo or prurigo. Diagnosis is easily confirmed by the parasitology smear, but in endemic areas the diagnosis is established on clinical examination.
The standard treatment in our study was intralesional meglumine antimoniate. The World Health Organization recommends one intralesional injection of 1-3 ml repeated at 2-day intervals until complete decoloration of affected tissues is achieved [13]. Some authors recommend the injection of 1-2 ml at four edges of the lesion, once or twice a week during a period of 3-6 consecutive weeks [14, 15]. In our opinion, this regimen is too painful and constraining for children. We use the treatment regimen of one local injection per week with further control within a month. This regimen leads to healing of nodular lesions with an average of 1.9 treatments. Intramuscular meglumine antimoniate was prescribed in case of resistance to local treatment, multiplicity of the lesions (over 5), and proximity to cartilage. Our patients received 60mg/kg/day with no side effects. Some authors report the success of using 30 mg/kg/day in childen in order to prevent cardiac side effects [16].
In conclusion, childhood cutaneous leishmaniais is frequent in our study. It has the characteristic of sporadic leishmaniasis. Mucosal leishmaniasis has a favorable outcome with neither destruction nor mutilations. The standard of therapy remains intralesional meglumine antimoniate using a protocol based on one local injection per month. This regimen has led to satisfactory results in our patients but further prospective studies are needed.
References
1. Chaffai M, Ben Rachid S, Ben Ismail R, Ben Osman A, Makni N. Formes clinico-épidémiologiques des leishmanioses cutanées en Tunisie. Ann Dermatol Venereol. 1988 ;115(12): 1255-1260. PubMed.2. Belhadj S, Djaiet-Baraket Z, Jemli B, Ben Osman A, Chaker E. Leishmanioses viscérales et cutanées du nord. Etude rétroactive des cas diagnostiqués à l’hôpital La Rabta de Tunis. Bull Soc Path Ex. 1996 ; 89(4) : 269-73. PubMed.
3. Gharbi Md-R, Ben Said A. Leishmanioses cutanées. Méd et Hyg. 1986;44:745-54. 4. Grevelink S A, Lerner EA. Leishmaniasis. J Am Acad Dermatol. 1996 Feb;34 (2Pt1):257-72. PubMed.
5. Marty P, Lacour JP, Pratlong F, Perrin C, del Giudice P, Le Fichoux Y. Leishmaniose cutanée localisée due à leishmania infantum MON-I contractée dans le nord de l’Algérie. Bull Soc Path Ex. 1998 ;91 :146-7. PubMed.
6. Guillet MH, Guillet G, Sassolas B, Leroy JP, Grosshans E, Calligaris D. Leishmaniose cutanée de l’enfant : Leishmanioe autochtone des aéroports ou leishmaniose meditérranné d’incubation prolongée? Nouv Dermatol. 1991 ;10 :454-5.
7. Di Rocco M, Vignola S, Borrone C, Rampini P, Occella C, Gambini C. Cutaneous leishmaniasis in a 6-month-old girl. J Pediatr 1998. Apr;132(4):748. PubMed 8. Sangueza OP,Sangueza JM, Stiller MJ, Sangueza P. Mucocutaneous leishmaniasis: A clinico-pathologic classification. J Am Acad Dermatol 1993. Jun;28(6):927-32. PubMed.
9. Berman JD. Human leishmaniasis: clinical, diagnostic and chemotherapeutic developments in the last 10 years. Clin Infect Dis. 1997Apr;24(4):684-703. PubMed.
10. Samady JA, Janniger CK, Schwartz RA. Cutaneous and mucocutaneous leishmaniasis. Cutis. 1996;57(1):13-20. PubMed.
11. Osorio LE, Castillo CM, Ochoa MT. Mucosal leishmaniasis due to leishmaniasis (viannia) panamensis in Colombia : Clinical characteristics. Am J Trop Med Hyg. 1998 Jul;59(1):49-52. PubMed.
12. Kharfi M, B. Fazaa, Chaker E, Kamoun MR. Mucosal localization of leishmaniasis in Tunisia: 5 cases. Ann Dermatol Venereol. 2003 Jan;130(1 Pt 1):27-30. PubMed.
13. No authors listed. Control of the leishmaniases. Report of a WHO Expert Committee. World Health Organ Tech Rep Ser. 1990;793:1-158. PubMed.
14. Sharquie KE, Al-Talib KK, Chu AC. Intralesional therapy of cutaneous leishmaniasis with sodium stibiogluconate antimony. Br J Dermatol. 1988 Jul;119(1):53-7. PubMed.
15. Moskowitz PF, Kurban AK. Treatment of cutaneous leishmaniasis. Retrospectives and advances for the 21th Century. Clin Dermatol. 1999 May-Jun;17(3):305-315. PubMed.
16. Selim MM, Vlasin Z, Jaroskova L. Leishmaniasis. Currently recommended treatment. Int J Dermatol. 1990 Jun;29(5):318-21. PubMed.
© 2004 Dermatology Online Journal

