Cutaneous Rosai-Dorfman disease: A case report
Published Web Location
https://doi.org/10.5070/D30x26t8rmMain Content
Cutaneous Rosai-Dorfman disease: A case report
Eden Pappo BA, Adrienne Schupbach MD, Sophie M Worobec MD
Dermatology Online Journal 18 (11): 6
University of Illinois Hospital & Health Sciences System, Chicago, IllinoisAbstract
A 40-year-old female presented with a 2-year history of asymptomatic nodules on her lower extremity. Symptoms began with a small dark spot on the right thigh, which progressively enlarged. She then developed similar nodules on her right leg and a lesion on her left buttock. On physical exam, her right proximal lateral thigh revealed a 10 cm x 6 cm indurated, pink-brown, heterogeneous plaque with a hyperpigmented rim. A similar 8 cm x 4 cm indurated plaque was on the distal right thigh. There was also a 3 to 4 cm hyperpigmented, thin plaque on the left posterior lower extremity and on the left inferior lateral buttock. Exam revealed no cervical or supraclavicular lymphadenopathy or organomegaly. Preliminary work-up by her primary physicians included serology for Lyme disease, systemic lupus erythematous, thyroid function tests, blood cultures for mycobacteria, and angiotensin-converting enzyme, which were all negative or within normal limits. Biopsies demonstrated a nodular inflammatory infiltrate within the dermis consisting of histiocytes with local aggregates of plasma cells and lymphocytes. Histiocytes were enlarged with vesicular nuclei. Some plasma cells had prominent Russell bodies, and emperipolesis was observed. Histiocytes stained positively for S-100, CD68 and CD45, while CD1A, CD30, and CD21; microorganism stains were negative.
Introduction
A 40-year-old female presented with a 2-year history of asymptomatic nodules on her lower extremity. Symptoms began with a small dark spot on the right thigh, which progressively enlarged. She then developed similar nodules on her right leg and a lesion on her left buttock. Her past medical history included diabetes mellitus (type II), hypertension, hyperlipidemia, and sleep apnea; she had been taking medications for these conditions.
Physical exam
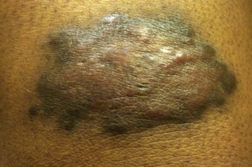
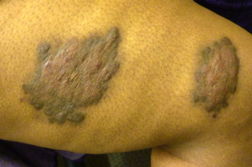
On physical exam, her right proximal lateral thigh revealed a 10 cm x 6 cm indurated, pink-brown, heterogeneous plaque with a hyperpigmented rim. A similar 8 cm x 4 cm indurated plaque was on the distal right thigh.
 |  |
| Figure 1 | Figure 2 |
|---|---|
| Figures 1 and 2. Gross images of lesion of Cutaneous Rosai-Dorfman Disease | |
There was also a 3 to 4 cm hyperpigmented, thin plaque on the left posterior lower extremity and on the left inferior lateral buttock. Exam revealed no cervical or supraclavicular lymphadenopathy or organomegaly. Skin biopsies from the left buttock and right thigh were obtained. Preliminary work-up by her primary physicians included serology for Lyme disease, systemic lupus erythematous, thyroid function tests, blood cultures for mycobacteria, and angiotensin-converting enzyme, which were all negative or within normal limits. After a final diagnosis, the patient declined further treatment.
Microscopic findings
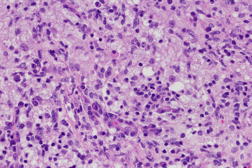
Three biopsies of the lesions demonstrated a nodular inflammatory infiltrate within the dermis consisting of histiocytes with local aggregates of plasma cells and lymphocytes.
 |
| Figure 5 |
|---|
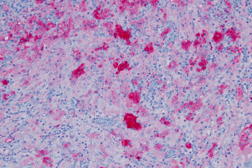
| Figure 5. S-100 staining of histiocytes typical of Cutaneous Rosai-Dorfman Disease (x20) |
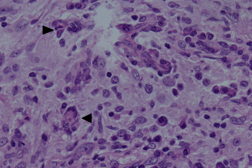
In all three specimens, histiocytes were enlarged with vesicular nuclei. Some of the plasma cells had prominent Russell bodies. Emperipolesis was noted as well with inflammatory cells seen within histiocytes.
Histiocytes stained positively for S-100, CD68 and CD45, whereas CD1A, CD30, and CD21 were negative. Microorganism studies including Periodic acid Schiff staining and Gomori silver stains (for fungal elements), Warthin-Starry staining (for spirochetes), and the Fite stain (for mycobateria) were negative.
Discussion
Rosai-Dorfman Disease (RDD) is also referred to as sinus histiocytosis with massive lymphadenopathy. RDD is rare, benign, and self-limited and is a non-Langerhans proliferative disorder of histiocytes [1]. The cellular changes are mainly within lymph nodes but spread to extranodal sites as well. Cervical lymphadenopathy is the most common clinical finding and is often accompanied by fever, leukocytosis (specifically neutrophilia), and polyclonal gammaglobulinemia [1].
The skin is the most common extranodal site. However when the disease is confined to the skin it is classified as cutaneous Rosai-Dorfman disease (CRDD). Patients with RDD tend to be young, male adults, whereas CRDD patients are typically older females and white. Asians are affected more commonly than black patients [2, 3]. Only 3 percent of cases of RDD are limited to cutaneous or subcutaneous findings and the lesions have variable forms, ranging from single papules to multiple nodules and plaques; any part of the body may be affected [2, 4].
Histologic features include dermal histiocytes and aggregates of lymphocytes and plasma cells. Histiocytes show positive staining for CD68 and S-100 and negative staining for CD1A. Emperiopolesis, phagocytosis of inflammatory cells, is common. Predominantly lymphocytes are seen within histiocyte cytoplasm.
The clinical presentation of CRDD is not well-described because of the rarity and variability in cutaneous findings. Lesions have been reported as erythematous, hyperpigmented, pruritic, and asymptomatic. They may be located on the extremities, back, within the ear, or even on the mons pubis [2, 5, 6]. Erythrocyte sedimentation rate may be a recommended laboratory exam, but is non-specific. RDD not limited to cutaneous findings may have an autoimmune component; immune disorders are found in 13 percent of patients [7]. No similar association with immune diseases has yet been described for CRDD.
Both RDD and CRDD are self-limited and benign, but treatment options are not well-defined. CRDD may be treated by surgical removal of the lesion, but recurrence after excision has been reported [8]. Alternative treatments include intralesional, topical, or systemic corticosteroids [3, 9]. Additionally, dapsone has been found to be effective and may be most beneficial in the presence of a neutrophil-predominant infiltrate [10]. Other treatments include imatinib, thalidomide, acitretin, isotretinoin, and cryotherapy [3, 11, 12].
References
1. Rosai J, Dorfman RF. Sinus histiocytosis with massive lymphadenopathy: a newly recognized benign clinicopathologic entity. Arch Pathol. 1969; 87:63-70. [PubMed]2. Brenn T, Calonje E, Granter SR, Leonard N, Grayson W, Fletcher CDM, et al. Cutaneous Rosai-Dorfman disease is a distinct clinical entity. Am J Dermatopathol. 2002;24:385-91. [PubMed]
3. Frater JL, Maddox JS, Obadiah JM, Hurley MY. Cutaneous Rosai-Dorfman disease: comprehensive review of cases reported in the medical literature since 1990 and presentation of an illustrative case. J Cutan Med Surg. 2006 Nov-Dec; 10(6):281-90. [PubMed]
4. Kong Y, Kong J, Shi D, Lu H, Zhu X, Wang J, et al. Cutaneous Rosai-Dorfman disease a clinical and histopathologic study of 25 cases in China. Am J Surg Pathol. 2007; 31: 341-50. [PubMed]
5. Tsang WY, Chan JK, Yu HC, Chow LT. Extranodal Rosai-Dorfman disease: an uncommon cause of persistent nodule in the ear. J Laryngol Otol. 1992;106:249-5. [PubMed]
6. Kang JM, Yang WI, Kim SM, Lee MG. Sinus histiocytosis (Rosai-Dorfman disease) clinically limited to the skin. Acta Derm Venereol. 1999;79:363-5. [PubMed]
7. Foucar E, Rosai J, Dorfman R. Sinus histiocytosis with massive lymphadenopathy: an analysis of 14 deaths occurring in a patient registry. Cancer. 1984; 54:1834. [PubMed]
8. Fening K, Bechtel M, Peters S, Zirwas M, Darabi K. Cutaneous rosai-dorfman disease persisting after surgical excision: report of a case treated with aceitretin. J Clin Aesthet Dermatol 2010;3(9): 34-6. [PubMed]
9. Salim A, Williamson M, Barker F, Hughes J. Steroid responsive cutaneous Rosai-Dorfman disease associated with uveitis and hypothyroidism. Clin Exp Dermatol. 2002 Jun;27(4):277-9. [PubMed]
10. Chan CC, Chu CY. Dapsone as a potential treatment for cutaneous Rosai-Dorfman disease with neutrophilic predominance. Arch Dermatol. 2006 Apr;142(4):428-30. No abstract available. [PubMed]
11. Gebhardt C, Averbeck M, Paasch U, Ugurel S, Kurzen H, Stumpp P, Simon JC, Treudler R. A case of cutaneous Rosai-Dorfman disease refractory to imatinib therapy. Arch Dermatol. 2009 May ;145(5): 571-4. [PubMed]
12. Tjiu JW, Hsiao CH, Tsai TF. Cutaneous Rosai-Dorfman disease: remission with thalidomide treatment. Br J Dermatol. 2003 May;148(5):1060-1. [PubMed]
© 2012 Dermatology Online Journal