Perioral dermatitis in a child associated with an inhalation steroid
Published Web Location
https://doi.org/10.5070/D30tq4z5z9Main Content
Letter: Perioral dermatitis in a child associated with an inhalation steroid
Praveen Kumar1 MD, Kalyan R Parashette MD1, Peter Noronha MD2
Dermatology Online Journal 16 (4): 13
1. Pediatric Resident, Department of Pediatrics, University of Illinois, Chicago, Illinois2. Associate Professor of Clinical Pediatrics, University of Illinois, Chicago, Illinois
Abstract
Perioral dermatitis, also known as periorificial dermatitis, is characterized by a papular rash involving the perioral, perinasal and periorbital areas of the skin. There are multiple agents that may cause these lesions, with topical steroids being the most common. Inhaled steroids are rarely implicated as a cause of perioral dermatitis. Our case is illustrative because there was a clear association of perioral dermatitis with the use of inhaled steroids and a quick response to the treatment regimen, which included discontinuation of the offending agent.
Introduction
Perioral dermatitis is an acneiform-like eruption, which commonly involves the perioral area. Mihan and Ayres coined the term ‘perioral dermatitis’ in 1964 [1]. In many cases, it is a reaction to topical steroids and other substances applied to the face. Discontinuation of these agents results in clearing. Oral tetracyclines and topical metronidazole application areusually effective.
Case
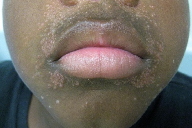
A 13-year-old boy was seen in the pediatric clinic complaining of “bumps on the face” for 1½ months. These lesions were first noticed underneath the chin and progressed to involve areas around the mouth and nose. Past medical history was significant for moderate persistent asthma. He was also reported to have atopic dermatitis when he was young, which had since resolved except for some hyperpigmentation of the antecubital areas. Asthma was diagnosed at 2 years of age and the patient was on varying regimens of bronchodilator and immunotherapy over the years. Two months before presenting with the eruption, he was placed on an increased dose of fluticasone / salmetrol (250 microgram / 50 microgram) by inhalation disc. During this period of time, there was no history of any other medication used on the face. On physical examination monomorphic pink papules were present in the peri-oral and nasolabial fold areas. Some hypopigmentation was also noticed. (Figure 1).
 |  |
| Figure 1 | Figure 2 |
|---|---|
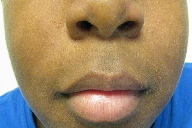
| Figure 1. Perioral dermatitis Figure 2. Clearance of dermatitis after discontinuation of inhaled steroids | |
A diagnosis of perioral dermatitis was made and was believed to be caused by inhaled steroids. This medication was discontinued and the patient was treated with doxycycline 50 mg twice per day along with alternating topicals of clindamycin 1 percent and metronidazole 0.75 percent. There was quick resolution and at two months follow up the perioral lesions had completely disappeared (Figure 2). In subsequent follow-ups there was no reoccurrence of the rash.
Discussion
Perioral dermatitis is a condition in which there are papular lesions most commonly around the mouth. This skin condition, albeit uncommon in childhood, has been reported in children from ages 7 months to 13 years; most are in the prepubertal period. Both the sexes are equally affected and no significant differences have been noted among different ethnic groups [2]. The rash is erythematous, papular, and papulopustular; the lesions predominantly involve the perioral area, but may also be perinasal and periorbiltal as well. Recently there has been a suggestion that this condition be named periorificial dermatitis because of the variable patterns of presentation around different orifices [3]. The cheeks are spared and other parts of the body are rarely involved. Multiple agents have been implicated as a cause for perioral dermatitis such as infectious agents, topical corticosteroids [4], fluorinated steroids [5], tartar control toothpastes [6], moisturizing creams [7], and inhaled steroids in asthmatic children [8, 9].
Our patient is a 13-year-old boy with known moderate persistent asthma on treatment with inhaled Fluticasone / Salmetrol. The perioral dermatitis cleared up rapidly after discontinuation of this inhaled medication. One of the theories for inhaled steroids causing perioral dermatitis is that the inhaled steroid gets deposited on the skin and has a direct local effect. In a large study of the local side effects, Dubus et al. has shown that approximately 3 percent of the children on inhaled steroids developed perioral dermatitis [8]. Yet there is only one other case report that relates the response to a specific regimen of treatment in the recent literature [9]. The patient’s history of asthma and atopic dermatitis suggest that this case of perioral dermatitis might be associated with atopy as previously suggested [10].
The histopathology is non-specific, with a variable perifollicular or perivascular lymphohistiocytic infiltrate [11] with occasional giant cells. The first step in treatment is discontinuation of inhaled steroids and substitution with another inhaled medication for asthma control. From the available literature it is unclear whether this causal relationship is steroid type specific or dose specific. Oral tetracyclines have been found to be veryeffective therapy along with metranidazole 0.75 percent topical application. The mechanism of action of metranidazole is unknown. In some cases, the rash can be prevented by oral rinsing and washing the perioral area with mild soap and water after each steroid inhalation [12].
In conclusion we believe that in our patient the perioral or periorificial dermatitis was clearly caused by inhaled steroids. The clinician should thus be aware of this potential complication of steroid inhaler use. Whether the rash could reoccur after reinstitution of the medication or substitution with another remains unclear.
References
1. Mihan R, Ayres S. Perioral dermatitis. Arch Dermatol 1964; 89:803-805 [PubMed]2. Laude TA, Salvemini JN. Perioral dermatitis in children. Semin Cutan Med Surg 1999;18:206-209 [PubMed]
3. Nguyen V, Eichenfield LF. Periorificial dermatitis in children and adolescents. J Am Acad Dermatol 2006;55:781-785 [PubMed]
4. Manders SM, Lucky AW. Perioral dermatitis in childhood. J Am Acad Dermatol 1992;27:688-692 [PubMed]
5. Cohen HJ. Perioral dermatitis. J Am Acad Dermatol 1981;4:739-740 [PubMed]
6. Ferlito TA. Tartar-control toothpaste and perioral dermatitis. J Clin Orthod 1992;26:43-44 [PubMed]
7. Kalkoff KW, Buck A. Etiology of perioral dermatitis. Hautarzt 1977;28:74-77 [PubMed]
8. Dubus JC, Marguet C, Deschildre A, et al. Local side-effects of inhaled corticosteroids in asthmatic children: influence of drug, dose, age and devise. Allergy 2001;56:944-948 [PubMed]
9. Held E, Ottevanger V, Petersen CS, Weismann K. Perioral dermatitis in children under steroid inhalation therapy. Ugeskr Laeger 1997;159:7002-7003 [PubMed]
10. Oehlschlaegel G, Schnabel P. Perioral dermatitis and the atopic constitution. Hautarzt 1979;30(10):532-536 [PubMed]
11. Wilkinson DS, Kirton V, Wilkinson JD, et al. Perioral dermatitis. Br J Dermatol 1979;101:245-257 [PubMed]
12. Poulos GA, Brodell RT. Perioral dermatitis associated with an inhaled corticosteroids. Arch Dermatol 2007;143(11):1460 [PubMed]
© 2010 Dermatology Online Journal

