Diagnosis of loxoscelism in two Turkish patients confirmed with an enzyme-linked immunosorbent assay (ELISA) and non-invasive tissue sampling
Published Web Location
https://doi.org/10.5070/D30th242g0Main Content
Diagnosis of loxoscelism in two Turkish patients confirmed with an enzyme-linked immunosorbent assay (ELISA) and non-invasive
tissue sampling
Sedat Akdeniz MD1, Jonathan A Green PhD2, William V Stoecker MD3, Hernan F Gomez MD4, S Ugur Keklikçi MD5
Dermatology Online Journal 13 (2): 11
1. University of Dicle, Faculty of Medicine, Department of Dermatology. sakdeniz@dicle.edu.tr2. Department of Animal Sciences,
University of Missouri-Columbia 3. The Dermatology Center, SpiderTech, Rolla MO 4. Department of Emergency Medicine, 1500
E. Medical Center Dr, Ann Arbor, MI 5. University of Dicle, Faculty of Medicine, Department of Opthalmology, Diyarbakır/TURKEYAbstract
Confirmed envenomations due to Loxosceles reclusa have not been previously documented in Turkey, to our knowledge. This brief report describes two Turkish patients with suspected envenomation by Loxosceles spider bites on the eyelids. Material obtained by swabbing the lesions with gauze was tested using a venom-specific enzyme-linked immunosorbent assay (ELISA). Both patients tested positive for the presence of Loxosceles venom.
Loxosceles reclusa and related arachnid species, indigenous to Europe as well as North America, are spiders that possess a venom capable of causing painful, disfiguring necrotic ulcers and, uncommonly, severe systemic effects [1, 2, 3, 4]. The diagnosis of a brown recluse spider bite is a clinical one made on the basis of the morphologic appearance of the cutaneous lesion [1, 2, 3, 4]. Definitive diagnosis is usually not possible because patients generally do not bring the offending spider to the clinician for identification. The morphology of a lesion is the usual basis for diagnosis but is not specific for Loxosceles spp. envenomation [3, 4, 5], as there are many mimics of spider bites [6, 7, 8].
For diagnostic confirmation of the two cases presented here, we utilized a sensitive and specific enzyme-linked immunosorbent assay (ELISA) designed to detect Loxosceles venom [9], using specimens obtained noninvasively by swabbing the lesions with cotton gauze.
Case 1
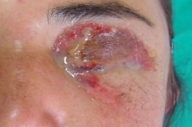
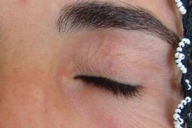
A 34-year-old Turkish woman who was on a sheep-dealing trip in the rural area of Siirt Turkey awoke in her tent with swollen, painful pruritic eyelids. She reported that she had seen spiders in her tent but the species was unknown. Within 3 days, massive facial edema developed, and a 2x3 cm hemorrhagic eyelid lesion with superficial necrosis was present, consistent with loxoscelism (Fig. 1). Upon hospital admission, she had a temperature of 38°C, with a pulse of 80 and blood pressure of 110/70 mm Hg. The results of the laboratory tests, including complete blood count, liver and renal function chemistries, urinalysis and coagulation functions, were all within normal limits. The lesion was managed with saline compresses and ocular lubrication. The lesion healed with resulting normal vision, normal eyelid function and no scarring (Fig. 2).
Case 2
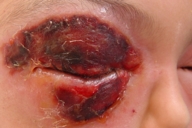
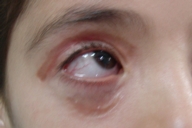
A 7-year-old girl from the rural area of Siirt Turkey awoke with pain, pruritus, and mild swelling of the eyelids. Within 3 days, severe bilateral eyelid edema was present. No spider was identified. On the third day, she was admitted to a hospital. A presumptive diagnosis of brown recluse spider envenomation was made, based on the appearance of the lesion. A painful, tender, hemorrhagic lesion showing early necrosis surrounded by severe facial edema was seen (Fig. 3). Upon hospital admission, she was normotensive with a temperature of 38°C, and a pulse of 100. She had a white blood cell count of 17,200 / µL with a significant left shift. Hemoglobin and hematocrit levels, urinalysis and other blood indices were within normal limits. The eyelid lesion was managed supportively with saline compresses and ocular lubricants. The lesion healed with scarring and visible hyperpigmentation (Fig. 4). Vision was normal and the eyelid could be opened fully. However, mild epiphora and punctuate epitheliopathy of the affected eyelid were observed. The child's parents observed that the right eyelid was incompletely closed when she slept.
Methods
All specimens for ELISA determination were obtained at the University of Dicle in Turkey. Gauze sponges soaked in normal saline were used to obtain a specimen from the affected lesions and contralateral control sites for both cases. The specimens were collected by gently swabbing the lesion and the control sites for 30 seconds. The swabs were taken on the 7th day after the onset of the lesion in Case 1 and on the 4th day after the onset of the lesion in case 2. Despite shipping by an express carrier, the shipments took 7 and 10 days and were stored in transit in ambient summertime temperatures for unknown durations. After shipment, the cotton samples were moistened with 300 µl ofTris buffered saline containing Tween-20 (20mM Tris pH8.0; 145 mM NaCl; 0.02% (v/v) Tween-20) and placed in a 0.5 cm diameter plastic centrifuge tube and centrifuged at 10,000g for 10 minutes to remove the saline from the absorbent material. Venom proteins in the solution were detected using an ELISA technique for detecting Loxosceles reclusa venom, originally described by Gomez et al. [9], with modifications noted herein.
Polyclonal capture and detection antibodies were raised in New Zealand white rabbits with unfractionated L. reclusa venom. Antibodies were purified from serum by means of protein A column liquid chromatography [10]. The concentration of blocking agents as noted in [9] was increased, nonfat milk solids were added to the blocking buffer, overnight incubation was used, and alkaline phosphatase was used as a detection agent. The generation of paranitrophenol product was monitored at 405 nm on a model ELx808, BIO-TEK, Inc. microplate reader. Separate standard curves were produced for each patient.
Results
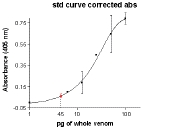
The contralateral control specimens all had absorbances at background level. The swab material from both cases showed venom immunoreactivity significantly greater than background signal, as shown in Figs. 5 and 6. These results are consistent with the presence of venom from a spider within the Loxosceles genus within the samples obtained with gauze from the lesions.
Discussion
Eyelid brown recluse bites are quite uncommon [12, 13, 14]. Severe edema is generally observed. Acute complications include elevated intraocular pressure [12] and airway compromise associated with laryngeal swelling [14]. Long-term complications include necrosis and scarring of the eyelid, which can lead to corneal irritation [13]. Therapeutic interventions for eyelid brown recluse bites have included dapsone, systemic corticosteroids, hyperbaric oxygen [12, 13], and debridement of necrotic tissue with flap reconstruction [14]. Cantharotomy and cantholysis have been used to restore normal pressure in a case with elevated intraocular pressure [12]. Supportive therapy can include topical and systemic antibiotics, saline dressings, and ocular lubricants. A bandage lens has been employed to minimize corneal irritation [13]
Controlled human trials supporting specific interventions for eyelid brown recluse bites are not available. One study showed benefit from a combination of dapsone and antivenom in experimental eyelid lesions in rabbits [15] However, another rabbit study reported no benefit from dapsone therapy for clinical outcome in skin lesions induced in rabbits. [16]. Edwards et al. noted that "caution must be emphasized to avoid the overzealous debridement of eyelid tissue. Because of the excellent blood supply, the eyelids. . .[have] a remarkable propensity for self-repair in the setting of gangrenous lid involvement." [14]
Although lesions attributed to Loxosceles rufescens have been reported from Turkey [17] and nearby areas around the Mediterranean [18], none of these reported spider bites were confirmed by identification of the spider known to have caused the bite. Loxosceles rufescens (Dufour, 1820) is established in Turkey [19] and is known to cause necrotic lesions. [20]
The massive eyelid edema and early necrosis observed in the two cases presented here are consistent with loxoscelism but not diagnostic, as other conditions, particularly envenomations from other arthropods, can have such a presentation. The venom ELISA provided supporting evidence for the diagnosis. Conservative management in the two cases reported here allowed both patients to heal without vision impairment, although one patient had residual functional impairment.
The degree of sensitivity and specificity of the ELISA for Loxosceles venom reported here has not been established in clinical cases. In vitro, the ELISA was found to be specific for Loxosceles species at relevant antigen levels, reacting to none of 17 other arthropod venoms at 40 ng [9]. In vivo, necrotic and inflammatory lesions that were tested with the ELISA had absorbances at the background level with this assay. This ELISA is not able to discriminate among Loxosceles species, which possess several common protein bands on western blot and display marked antigenic cross-reactivity. [11]
In summary, the polyclonal swab ELISA assay performed on material obtained by cotton gauze allowed identification of Loxosceles venom upon the skin, 4-7 days after the onset of symptoms in the two bites reported here, supporting the diagnosis of Loxosceles envenomation by a spider of the Loxosceles genus in two Turkish patients.
Acknowledgment: The assistance of Tina Parks in protein preparations and ELISA determinations is gratefully acknowledged.
References
1. Atkins JA, Wingo CW, Sodeman WA, Flynn JE. Necrotic arachnidism. Am J Trop Med Hyg 1958; 7:165-184. PubMed2. Wasserman GS, Anderson PC, Loxoscelism and necrotic arachnidism. J Toxicol Clin Toxicol 1983-1984; 21:451-472. PubMed
3. Sams HH, Dunnick CA, Smith ML, King LE Jr. Necrotic arachnidism. J Am Acad Dermatol 2001; 44:561-573. PubMed
4. Anderson, PC. Spider bites in the United States. Dermatol. Clin 1997; 15(2):307-311. PubMed
5. Vetter RS. Envenomation by a spider, Agelenopsis aperta (family: Agelenidae) previously considered harmless. Ann Emerg Med 1998; 32:739-741. PubMed
6. Rosenstein ED, Kramer N. Lyme disease misdiagnosed as a brown recluse bite [letter]. Ann Intern Med 1987; 107:782. PubMed
7. Rees R, Campbell D, Rieger E, King LE. The diagnosis and treatment of brown recluse spider bites Ann Emerg Med. 1987; 16:945-949. PubMed
8. Moaven LD, Altman SA, Newnham AR. Sporotrichosis mimicking necrotising arachnidism. Med J Aust. 1999; 171:865-868 PubMed
9. Gomez HF, Krywko DM, Stoecker WV. A new assay for the detection of Loxosceles species (brown recluse) spider venom. Ann Emerg Med 2002; 39(5):469-74. PubMed
10. Harlow E, Lane D. Antibodies: A laboratory manual. 1988; Cold Spring Harbor Laboratory.
11 . Gomez HF, Miller MJ, Waggener MW, Lankford HA, Warren JS. Antigenic cross-reactivity of venoms from medically important North American Loxosceles spider species. Toxicon 2001; 39(6):817-24. PubMed
12. Jarvis RM, Neufeld MV, Westfall CT. Brown recluse spider bite to the eyelid. Ophthalmology 2000 Aug; 107(8):1492-6. PubMed
PubMed [PubMed - indexed for MEDLINE]
13. Wesley RE, Ballinger WH, Close LW, Lay AM. Dapsone in the treatment of presumed brown recluse spider bite of the eyelid. Ophthalmic Surg 1985; 16(2):116-7, 120. PubMed
14. Edwards JJ, Anderson RL, Wood JR. Loxoscelism of the eyelids. Arch Ophthalmol 1980; 98(11):1997-2000. PubMed
15. Cole HP 3rd, Wesley RE, King LE Jr. Brown recluse spider envenomation of the eyelid: an animal model. Ophthal Plast Reconstr Surg 1995; 11(3):153-64.
16. Elston DM, Miller SD, Young RJ 3rd, Eggers J, McGlasson D, Schmidt WH, Bush A. Comparison of colchicine, dapsone, triamcinolone, and diphenhydramine therapy for the treatment of brown recluse spider envenomation: a double-blind, controlled study in a rabbit model. Arch Dermatol 2005; 141(5):595-7. PubMed
17. Atilla R, Cevik AA, Atilla OD, Yanturali S. Clinical course of a loxosceles spider bite in Turkey. Vet Hum Toxicol 2004; 46(6):306-8. PubMed
18. Borkan J, Gross E, Lubin Y, Oryan I. An outbreak of venomous spider bites in a citrus grove. Am J Trop Med Hyg 1995; 52(3):228-30. PubMed
19. http://www1.gantep.edu.tr/~varol/eng/posionous accessed November 6, 2006.
20. Young AR, Pincus SJ. Comparison of enzymatic activity from three species of necrotising arachnids in Australia: Loxosceles rufescens, Badumna insignis and Lampona cylindrata. Toxicon 2001; 39(12):1941-3. PubMed
© 2007 Dermatology Online Journal