Frontal fibrosing alopecia
Published Web Location
https://doi.org/10.5070/D30s33h12tMain Content
Frontal fibrosing alopecia
Lesley Clark-Loeser MD, and Jo-Ann Latkowski MD
Dermatology Online Journal 11 (4): 6
Department of Dermatology, New York University School of Medicine
Abstract
A 75-year-old woman presented with a 3-year history of progressive loss of her eyebrow hair and with frontal-parietal hairline recession. Multiple biopsy specimens supported a histopathologic diagnosis of lichen planopilaris. With these histolopathologic findings, and the patient's clinical presentation, a diagnosis of frontal fibrosing alopecia was made. Treatment to date with topical glucocorticoid preparations, intralesional triamcinolone injections, and tacrolimus ointment have been unsuccessful.
A 75-year-old woman was seen for a 3-year history of hair loss involving the scalp and eyebrows. The patient initially presented to a dermatologist in March 2004 with the complaint of hair loss of her eyebrows and bumps along her frontal hairline. At that time a biopsy specimen obtained from the frontal hairline was interpreted as a perifolliculitis. Over the next year, the patient continued to lose eyebrow hair and complained of increased inflammation along her frontal hairline and of newly noted frontal hairline recession. She was treated with intralesional triamcinolone injections, multiple topical glucocorticoid preparations, and tacrolimus ointment without benefit. The patient was referred to NYU Dermatology Associates for further evaluation in January 2005, and an additional biopsy was obtained. Past medical history includes non-insulin-dependent diabetes mellitus, rosacea, basal-cell carcinoma, and breast cancer for which she underwent a mastectomy.
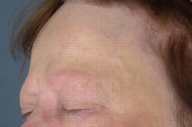
There was complete loss of eyebrow hair. The frontal-parietal hair line was recessed with perifollicular edema and mild follicular hyperkeratosis.
|
|
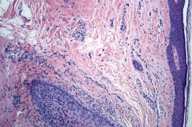
| Figure 1 | Figure 2 |
|---|
A complete blood count, complete metabolic panel, and thyroid function panel were normal.
Histopathology reveals a reduced number of hair follicles with a lichenoid, perifollicular, lymphocytic infiltrate and peri-infundibular fibroplasia.
Comment:
First described in 1994, postmenopausal frontal fibrosing alopecia (FFA) displays prominent frontal and frontal-parietal hairline recession, often with concomitant thinning or complete loss of the eyebrows [1]. Almost all reported cases have occurred in women who are postmenopausal [2].
This form of scarring alopecia requires clinical pathologic correlation in order to make the diagnosis. Women with this condition typically present with the complaint of asymptomatic, progressive recession of their frontal hairline. Clinical examination shows symmetric, marginal alopecia along the frontal and frontal-parietal hairline. Most often, the affected scalp skin is pale and smooth with loss of follicular orifices; however, perifollicular erythema and follicular keratinization also may be observed [3].
Histopathologic examination of affected scalp shows a reduced number of hair follicles, which have been replaced by fibrous tracts, and a lymphocytic infiltrate in a lichenoid pattern about the infundibular, isthmus, and bulge portions of the remaining follicles. This perifollicular, lymphocytic, lichenoid inflammation is typical of lichen planopilaris, and FFA is considered to be a variant of lichen planopilaris [4].
Additional evaluation of these patients may include a complete blood count, a thyroid function panel, androgens, erythrocyte sedimentation rate, antinuclear antibody, and antibodies to double-stranded DNA and extractable nuclear antigen. Most often, these laboratory investigations are normal [4].
No treatments have been found to alter the course of frontal fibrosing alopecia. Treatments that have been employed include oral prednisone (25-50 mg/day), chloroquine phosphate (150 mg/day), moderate potency topical glucocorticoid preparations, intralesional glucocorticoids, topical retinoic acid, minoxidil 2 percent solution, oral isotretinoin (50 mg/day), and ultramicronized griseofulvin (330 mg/day) [4]. Hormone replacement therapy does not appear to alter the development or progression of this condition [4].
References
1. Kossard S. Postmenopausal frontal fibrosing alopecia, scarring alopecia in a pattern distribution. Arch Dermatol 1994;130: 770. PubMed2. Tosti A, Piraccini BM, Iorizzo M, Misciali C. Frontal fibrosing alopecia in postmenopausal women. J Am Acad Dermatol. 2005 Jan;52(1):55-60. PubMed
3. Kossard S, Lee MS, Wilkinson B. Postmenopausal frontal fibrosing alopecia: a frontal variant of lichen planopilaris. J Am Acad Dermatol. 1997 Jan;36(1):59-66. PubMed
4. Olsen EA, Bergfeld WF, Cotsarelis G, Price VH, Shapiro J, Sinclair R, Solomon A, Sperling L, Stenn K, Whiting DA, Bernardo O, Bettencourt M, Bolduc C, Callendar V, Elston D, Hickman J, Ioffreda M, King L, Linzon C, McMichael A, Miller J, Mulinari F, Trancik R; Workshop on Cicatricial Alopecia. Summary of North American Hair Research Society (NAHRS)-sponsored Workshop on Cicatricial Alopecia, Duke University Medical Center, February 10 and 11, 2001. J Am Acad Dermatol. 2003 Jan;48(1):103-10. PubMed
© 2005 Dermatology Online Journal

