Docetaxel-induced supravenous serpentine dermatitis
Published Web Location
https://doi.org/10.5070/D309m643s1Main Content
Letter: Docetaxel-induced supravenous serpentine dermatitis
Sudip Kumar Ghosh MD DNB1, Debabrata Bandyopadhyay MD1, Loknath Ghoshal MD1, Swapnendu Basu MD DNB2
Dermatology Online Journal 17 (11): 16
1. Department of Dermatology, Venereology, and Leprosy2. Department of Radiotherapy
R G Kar Medical College, Kolkata, India. dr_skghosh@yahoo.co.in
Abstract
Serpentine erythematous or hyperpigmented streaks along the superficial venous network proximal to the site of injection may occur as a distinctive eruption after infusion of several chemotherapeutic agents. This morphological pattern has been described under various terms like, "persistent supravenous erythematous eruption," "persistent serpentine supravenous hyperpigmented eruption," or "persistent serpentine supravenous hyperpigmentation." These changes belong to the same clinical spectrum, which most often starts as erythematous serpentine streaks precisely located over the injected veins; the erythema is shortly replaced by hyperpigmentation. We report here a case of docetaxel-induced supravenous serpentine dermatitis with some interesting clinical and histological features.
Introduction
Treatment with intravenous chemotherapeutic agents may be associated with a wide gamut of cutaneous adverse effects. Erythematous or hyperpigmented linear streaks along the superficial venous network proximal to the site of injection have been reported after infusion of several chemotherapeutic agents [1]. The terms "persistent supravenous erythematous eruption" (PSEE), "persistent serpentine supravenous hyperpigmented eruption" (PSSHE), and "persistent serpentine supravenous hyperpigmentation" have been used to describe this condition. This group of cutaneous disorders is thought to represent a clinical spectrum that most often starts as erythematous serpentine streaks precisely located over the injected veins, followed by hyperpigmentation [2]. We report here a case of docetaxel-induced supravenous serpentine dermatitis for its relative rarity and interesting clinical and histological features.
Case report
 |  |
| Figure 1 | Figure 2 |
|---|
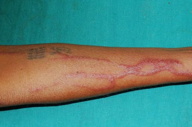
A 45-year-old woman, a patient with recurrent breast carcinoma, was scheduled for chemotherapy with docetaxel 100 mg/m² cycled every 21 days. The first dose was infused through a peripheral intravenous cannula in the left forearm. The patient had premedication with oral dexamethasone (8 mg twice daily) and ondensetron (8 mg twice daily), started one day prior to chemotherapy and continued for three more days. Intravenous doses of ranitidine (50 mg), pheniramine maleate (50 mg), and ondansetron (16 mg) were administered (in the right forearm) half an hour prior to the infusion. On the next day the patient developed a burning sensation and mild itching over the left forearm. She noticed a red line spreading along the path of infusion of the chemotherapeutic agent. Over the next few days, the itching intensified and the rash spread further proximally. There were no constitutional symptoms. Examination revealed an erythematous, branched, slightly scaly, non-tender, serpiginous skin eruption, which traced its path along the superficial venous network of the left forearm. A few excoriations were also noted (Figure 1). There were no other mucocutaneous lesions or regional lymphadenopathy.
 |  |
| Figure 3 | Figure 4 |
|---|
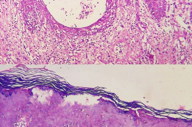
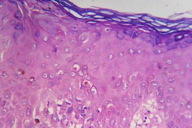
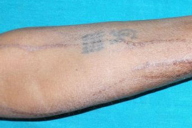
Complete hemogram and routine biochemistry were normal. A lesional skin biopsy was performed on the 7th day of the appearance of the skin lesions. Histopathological examination revealed a basket-weave pattern of hyperkeratosis, spongiosis with lymphocytic and neutrophilic exocytosis, irregular acanthosis, focal basal cell degeneration, upper dermal band-like as well as perivascular lympho-mononuclear infiltrates, and papillary dermal edema (Figures 2 and 3). Based on the clinical and histopathological features, a diagnosis of docetaxel-induced supravenous serpentine dermatitis was made. The patient was prescribed mometasone furoate (0.1%) ointment once daily for a period of 2 weeks. The skin lesions showed significant improvement within a week (Figure 4).
Discussion
Serpentine supravenous hyperpigmentation has been observed in patients treated with several chemotherapeutic agents [1-5], such as nitrogen mustard, nitrosoureas, cyclophosphamide, fotemustine, actinomycin, doxorubicin, vinca alkaloids, vinorelbine, taxanes, docetaxel, proteasome inhibitors, bortezomib, and different combinations of chemotherapeutic agents. Although the precise pathological mechanism is currently unknown, the most probable explanation is a direct cytotoxic effect of the agents on the vascular endothelium [4].
Histopathologically, persistent supravenous eruption may show an interface dermatitis with isolated necrotic keratinocytes, papillary dermal edema, and superficial perivascular inflammatory infiltrates [2]. However, features of both spongiotic and interface dermatitis were observed in our patient. Based on the morphology of the skin dyspigmentation, the clinical differential diagnosis should include thrombophlebitis, cutis marmorata, erythema ab igne, livedo reticularis, and lichen planus running along superficial cutaneous veins [3]. Unlike tender, clot-forming thrombophlebitis, the underlying vessels of serpentine supravenous hyperpigmentation remain patent [5]. Each of these diagnoses can be readily excluded from the history and thorough clinical examination. Physicians should be aware of this distinctive cutaneous effect of chemotherapeutics owing to their widespread use in the treatment of malignancies.
References
1. Aydogan I, Kavak A, Parlak AH, Alper M, Annakkaya AN, Erbas M. Persistent serpentine supravenous hyperpigmented eruption associated with docetaxel. J Eur Acad Dermatol Venereol 2005; 19:345-7. [PubMed]2. Mataix J, Betlloch I, Palmero F, Romero A. Persistent supravenous eruption induced by intravenous bortezomib therapy. Br J Dermatol 2008; 158:863-4. [PubMed]
3. Geddes ER, Cohen PR. Antineoplastic agent-associated serpentine supravenous hyperpigmentation: superficial venous system hyperpigmentation following intravenous chemotherapy. South Med J 2010; 103:231-5. [PubMed]
4. Jain V, Bhandary S, Prasad GN, Shenoi SD.Serpentine supravenous streaks induced by 5-fluorouracil. J Am Acad Dermatol 2005; 53:529-30. [PubMed]
5. Chan CC, Lin SJ. Images in clinical medicine. Serpentine supravenous hyperpigmentation. N Engl J Med 2010 29; 363:e8. [PubMed]
© 2011 Dermatology Online Journal

