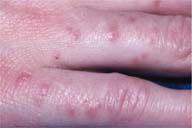

Cactus dermatitis is a common problem among harvesters of cactus fruit. The smaller spines (glochidia) are responsible for most of the dermatitis. Easily separated from the body of the plant, the glochidia may be transferred to bystanders through contact with clothing or pets exposed to these cacti. Removal of the glochidia from the skin is key to treatment, and household glue may aid in this extraction.
Cacti are dicotyledonous (characterized by two seed leaves) flowering plants belonging to the family Cactaceae. These succulent perennial plants are native through most of the length of North and South America, especially the dry regions. Cacti generally have thick herbaceous or woody chlorophyll-containing stems. In most species, leaves are absent and the stem performs the photosynthetic functions of the plant.
There are approximately 2000 species and 100 genera of cacti are located primarily in the drier regions of tropical and subtropical America. These plants have been exported to many other areas, and thrive in the Mediterranean region, India, Africa, and Australia. In addition, they have become popular indoor plants in areas where they are not native.[1]
Cacti are characterized by the presence on the surface of areoles, nipple or cushion-like structures. In most species of cacti, spines or bristles arise from the areoles. The presence of areoles distinguishes these spiney plants from another family of spiny succulents, Euphorbiaceae.
Opuntiais the largest genus of the cactus family. This genus is characterized by the presence of tufts of short barbed hairs, glochidia, that arise from the areoles. Within the Opuntia genus are subgoups based on the form of the stem segments. The chollas are characterized by cylindrical joints. Prickly pears are characterized by flat joints.
Cholla is the subgoup of the Opuntia genus characterized by cylindrical joints. These plants are also known as Jumping Cactus or Jumping Cholla, because of the disconcerting habit of coming unjointed easily. Simply touching a spine is enough to detach a joint. If a spine become lodged in the skin, movement may result in further detachment and additional joints becoming lodged in the skin. To make matters worse, the spines are barbed and therefore difficult to remove.
The Sabra or Indian fig (Opuntia gymnocarpa) is known for the occupational dermatitis in harvesters of the succulent fruit. Native to Mexico, this plant is now worldwide and frequently cultivated for the edible fruit.
The dermatitis that occurs from contact with cacti is primarily mechanical or irritant, although immunologic and infectious reactions can also occur. Contact with the spines can scratch the skin or induce wounds and multiple excoriations. The spines may break off in the skin or subcutaneous tissue resulting in papules or nodules. Presence of the spines within the skin may evoke a granulomatous response.
While the larger spines may appear menacing, actually more problems appear to result from skin penetration and retention of the glochidia. These minute structures may be barbed and once they have penetrated the skin they are difficult to dislodge. Implanting glochidia in the skin is noted to produce immediate irritation. This may not always occur, as suggested by the presentation of patients with the later (granulomatous lesions around glochidia) who have no recollection of the acute injury. In some cases, the irritant reaction may have a delayed onset. Shanon reported that brushing his axillary skin with sabra fruit resulted in no symptoms for a half hour, followed by 1 1/2 hours of "stabbing feelings".[2] Winer reports immediate burning sensation, redness and swelling which remained for one to three days if the spines were removed.[3] Depending on the exposure, widespread areas may be involved, even extending to hard palate, tongue, conjunctiva and cornea.[2]
If the glochidia are not removed, a response may ensue that eventuates in granulomatous dermatitis. Within 24 to 72 hours there is the appearance of 2- to 5-mm, asymptomatic, domed, glistening papules, sometimes erythematous, with a central pin-point-sized black dot at the site of the injury.[4] There may be groups of these papules. Vesicles and pustules and even focal ulceration may also occur.[2] In some instances, diagnosis can be made easily by passing the fingers over the affected area and by feeling the embedded glochidia.[2]
Left untreated, these lesions may last as long as 9 months. A biopsy of the later lesions reveals granuloma formation with plant material embedded in the dermis. The fragments of the barbed bristles gave strongly positive reactions with PAS.[5] The presence of a cactus granuloma lesion is often followed by post-inflammatory hyperpigmentation.
The skin reaction of gatherers of the fruit was described in Israel and is known as "sabra dermatitis".[2] This condition is characterized by a papular or vesicular reaction that is sometimes scabies-like. It has also been described as tinea-like[6] and dyshidrosis-like.[7] The hard palate and tongue are occasionally affected.[8] Typical areas of involvement of this irritant dermatitis include fingers, wrists, genitals, thorax, and buttocks. Biopsy of these lesions will reveal that they contain glochidia. Glochidia may be transferred to the workers' clothing and thence to other individuals. It is recommended that the fruit should be picked only when wetted, and picking should be stopped when it is windy since the glochidia can become airborne.[8]
In addition to mechanical and irritant dermatitis, there are rare reports of infection arising from penetration of the cactus spines. Mycobacterium marinum infection has been reported.[9] Fungal and nocardia infection are also reported.[10] For the most part, cactus spine wound sites are culture negative.[11]
There is a discussion in the literature about the role of allergy in generation of the granulomatous response to cactus spine injury. Because injury with cactus spines appears to be common and the granulomatous response infrequent, Schreiber postulated that allergy was involved.[4] Evaluating six patients with cactus granulomas, they found positive immediate reactions in two of the six scratch tested and in five of the six intradermally injected patients. However, the argument against allergy is strengthened by the finding of foreign body rather than epitheliod granulomas.[4,12] Nevertheless, epithelioid granulomatous responses have been documented by others.
Of relevance as an occupational disease, true IgE-mediated allergy to cacti in workers handling cacti has been reported by Paulen. Both genetic predisposition and close contact with the plants seem to be important factors in determining IgE allergy.[13] In some individuals, contact urticaria and rhinitis appear to be related to exposure to cacti and correlate with positive skin prick testing.[14]
If the glochidia are allowed to remain in the skin, a dermatitis may ensue that will persist for months. It may help to treat the affected area with a topical corticosteroid.[15] However, since the presence of glochidia is the inciting factor, removal of these minute spines would seem to be a more rational approach.
Glochidia may be difficult to remove. Yanking out the bristles may result in leaving one or more 20 micron-30 micron sized barbs in the skin, later to be manifest by granuloma formation.[4] Attempts to suck out the glochidia are likely to result in their attachment to the tongue.[7] Popular methods of removing glochidia have included spreading adhesive plaster over the area and ripping it off quickly or using melted wax (hot wax sometimes employed for removing hair). Martinez et al.[16] studied various methods of removing glochidia from rabbit skin. They evaluated tweezers, glue, facial mask, adhesive tape, package-sealing tape, and tweezing followed by glue. The most effective single method was tweezing, which removed 76% of the spines. The method using a thin layer of household glue (Elmer's Glue-All, Borden Inc) covered with gauze, allowed to dry (about 30 minutes) and then peeled off resulted in removal of 63% of the spines. Facial mask and adhesive tapes removed about 40% and 30% of the spines, respectively, and produced more retention and inflammation three days after removal than no treatment. Repeated applications of adhesive tape did not improve the results. According to Martinez, the most effective method is to first use tweezers to remove clumps of spines followed by the application and removal of household glue, resulting in removal of 95% of the spines.
Unroofing the early vesicles or pustules may permit manual extraction of the spicules. Soaking unroofed papules may allow for extrusion of the glochidia. Faster resolution may be obtained by removing the papules. A method of treatment has been described for the granulomatous papules, and involves unroofing the granulomatous papules, removing the glochidia fragments under a dissecting microscope, and subsequent soaking the wound in an antibacterial solution.[17]
© 2001 Dermatology Online Journal