Successful Treatment of Eosinophilic pustular folliculitis with topical Tacrolimus 0.1 percent ointment
Published Web Location
https://doi.org/10.5070/D30jt2x1b1Main Content
Successful treatment of eosinophilic pustular folliculitis with topical tacrolimus 0.1 percent ointment
Shanna Shan-Yi Ng MRCP (UK), Yong-Kwang Tay FRCP (Lond)
Dermatology Online Journal 18 (2): 10
Department of Dermatology, Changi General Hospital, SingaporeAbstract
Classic eosinophilic pustular folliculitis (EPF), otherwise known as Ofugi disease, is a rare condition commonly treated with topical glucocorticosteroids. If this fails, oral indomethacin is frequently the next line. Because the condition is recurrent, the use of long term steroids may cause side effects such as skin atrophy, hypertrichosis, and dyspigmentation. Topical tacrolimus is an immunosuppressant that is generally used as a steroid-sparing agent in atopic dermatitis. We report a case of classic EPF, which was recurrent over 5 years that had failed topical glucocorticosteroids but was successfully treated with topical tacrolimus 0.1 percent ointment.
Case report
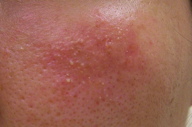 | 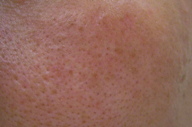 |
| Figure 1a | Figure 1b |
|---|
A 46-year-old woman presented with recurrent pruritic red plaques over the cheeks of 5 years duration. She first presented with a discrete pruritic red plaque over the right cheek in 2004 and was initially worked up for lupus erythematosus. Complete blood count, including the eosinophil count, erythrocyte sedimentation rate, anti-double stranded DNA, and anti-extractable nuclear antibody were normal or negative. Anti-nuclear antibody was 1:100. Betamethasone 0.1 percent valerate cream twice a day was prescribed. The patient subsequently failed to follow-up, but presented again in 2009 with a one-month history of a discrete pruritic red plaque, this time over the left cheek (Figure 1a). She was prescribed mometasone furorate 0.1 percent cream twice a day. Anti-nuclear antibody was repeated and was negative.
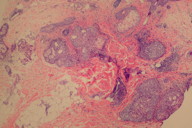 | 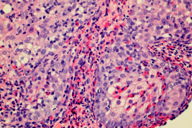 |
| Figure 2a | Figure 2b |
|---|
After a month of topical glucocorticosteroids, the plaque remained unchanged. Histopathology revealed a perivascular and periadnexal inflammatory infiltrate of lymphocytes and eosinophils. Eosinophils were seen in aggregates within the sebaceous lobules and hair follicles, which confirmed the diagnosis of EPF (Figures 2a and 2b). Significant improvement was noted after 2 weeks of topical tacrolimus 0.1 percent twice a day (Figure 1b), with resolution of the rash after 1 month and no recurrence after 7 months. There were no side effects noted.
Discussion
Eosinophilic pustular folliculitis (EPF) is a rare condition of unknown cause. A myriad of treatments are available for this condition and topical tacrolimus is not first line. The first choice tends to be topical corticosteroids, failing which the oral treatment with the best success rates is indomethacin [1, 2]. Other oral treatments used with varying success include prednisolone, retinoids, colchicine, dapsone, itraconazole, and metronidazole. Temporary improvement with UVB and psoralen plus UVA has also been reported [1].
The successful use of tacrolimus 0.1 percent ointment in this condition was first described by Dale [5]. Following this, there have only been a few case reports of successful treatment with tacrolimus 0.1 percent ointment noted in patients who have failed topical glucocorticosteroids, oral indomethacin, minocycline, and dapsone [3, 4, 6]. Especially for patients in whom indomethacin may be contraindicated because of gastrointestinal side effects, tacrolimus 0.1 percent ointment or pimecrolimus 1 percent cream maybe an effective and safe option [6, 7].
In a retrospective case series, Fukamachi et al had a patient who responded completely after tacrolimus 0.1 percent ointment was added to a combination of oral roxithromycin, loxoprofen sodium, and topical indomethacin. The redness and pustules resolved earlier but pruritus and papules only resolved after topical tacrolimus was subsequently added [8]. There have been no reports of any side effects in all case reports.
The response of EPF to tacrolimus may help shed some light on its pathogenesis. Tacrolimus causes immunosuppression by inhibiting the proliferation and activation of CD4+ T helper cells by binding to the cellular receptor known as FK506-binding protein (FKBP). The tacrolimus-FKBP complex then binds to calcineurin thus preventing the dephosphorylation of the nuclear factor of activated T cells and consequently, blocking the cascade of cytokine gene transcription [9].
We report this case to further substantiate the successful use of topical tacrolimus in EPF. Topical tacrolimus can be tried especially in those who fail topical corticosteroids and may be an alternative to oral indomethacin. With its increased usage in conditions other than atopic dermatitis, we believe it may soon be considered the treatment of choice, at least in EPF, in view of its rapid efficacy and safety. It is effective for intermittent short duration of use with low rates of recurrence.
References
1. Nevri SJ, Schwartz RA, Dmochowski M. Eosinophilic pustular folliculitis: A 40 year retrospect. J Am Acad Dermatol. 2006; 55:285-89. [PubMed]2. Tang M BY, Tan E, Chua SH. Eosinophilic pustular folliculitis (Ofugi’s disease) in Singapore: A review of 23 adult cases. Australasian J of Dermatol. 2003; 44:44-47. [PubMed]
3. Hara Dai, Kuroda K, Mieno H, Tajima S. Treatment of eosinophilic pustular folliculitis with tacrolimus ointment. J Am Acad Dermatol. 2004; 51:143-45. [PubMed]
4. Kawaguchi M, Mitsuhashi Y, Kondo S. Successful treatment of eosinophilic pustular folliculitis with topical tacrolimus. Int J of Dermatol. 2004; 43:608-10. PubMed]
5. Dale S, Shaw J. Eosinophilic pustular folliculitis (case report). Lancet. 2000; 356:1235. [PubMed]
6. Kabashima K, Sakurai T, Miyachi Y. Treatment of eosinophilic pustular folliculitis (Ofugi’s disease) with tacrolimus ointment. Br J of Dermatol. 2004; 151:949-50. [PubMed]
7. Rho NK, Kim BJ. Eosinophilic pustular folliculitis: successful treatment with topical pimecrolimus. Clin Exp Dermatol. 2007; 32:108-09. [PubMed]
8. Fukumachi S, Kabashima K, Sugita K et al. Therapeutic effectiveness of various treatments for eosinophilic pustular folliculitis. Acta Derm Venerol. 2009; 89:155-59. [PubMed]
9. Ruzicka T, Assmann T, Homey B. Tacrolimus: the drug for the turn of the millennium? Arch Dermatol. 1999; 135:574-80. [PubMed]
© 2012 Dermatology Online Journal

