Elastosis perforans serpiginosa in a patient with trisomy 21
Published Web Location
https://doi.org/10.5070/D35v58999vMain Content
Elastosis perforans serpiginosa in a patient with trisomy 21
Jeffrey S Newman MD, Maxwell A Fung MD
Dermatology Online Journal 12 (5): 5
University of California at Davis Department of Dermatology. jeffrey.newman@ucdmc.ucdavis.eduAbstract
A 12-year-old girl with trisomy 21 (Downs syndrome) presented with an approximate 2-year history of an asymptomatic eruption on the right upper arm and left lateral neck that was clinically and histologically diagnostic of elastosis perforans serpiginosa (EPS). EPS is a perforating dermatosis affecting the face, ear, neck, extremities, or trunk. It occurs with greater frequency in persons with trisomy 21, as well as some other genetic syndromes and after D-penicillamine therapy. It has also been reported as a sporadic, presumably unrelated disorder in several acquired diseases.
Clinical synopsis
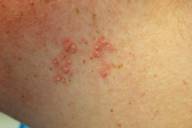
In July 2005 a 12-year-old girl with trisomy 21 presented to the University of California Davis Department of Dermatology for evaluation of a scalp lesion. The lesion was clinically consistent with a prurigo nodule and treatment was begun. However, in the course of the initial visit, additional lesions were noted on the right upper arm and the left lateral neck that were inconsistent with prurigo nodularis. Physical examination revealed additional lesions consisting of keratotic erythematous papules arranged in arcuate configurations on the right upper outer arm and the left neck (Fig. 1).
 |
| Figure 1 |
|---|
| Figure 1. Lateral aspect of the left neck |
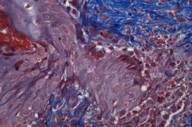
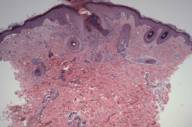
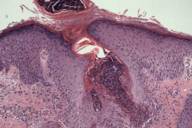
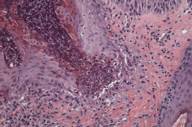
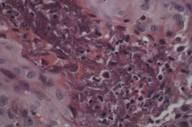
A biopsy was obtained from the left neck. Histopathological examination showed a focal area of epithelial acanthosis and canalization with overlying parakeratotic plugging. Basophilic nuclear debris and eosinophilic fibers are observed entering the epithelial channel from the underlying papillary dermis (Fig. 2a). Verhoef-van Gieson staining of sections highlighted the extruded dermal fibers, confirming their identity as elastin fibers (Fig. 3a). Trichrome stain demonstrated that blue-staining collagen fibers were not involved (Fig. 3b). Clinical and histopathological findings supported a diagnosis of EPS.
 |  |
| Figure 2A | Figure 2B |
|---|
 |  |
| Figure 2C | Figure 2D |
|---|---|
| Figures 2. Hematoxylin and eosin stained sections. A: Original magnification 40×. B: Original magnification 100×. C: Original magnification 200×. D: Original magnification 600× | |
Comment
Elastosis perforans serpiginosa is a disorder characterized by transepithelial elimination of elastin. It is a member of a larger class of perforating disorders that hold in common the transepithelial elimination of extracellular material or fibers from the dermis. The other perforating disorders are reactive perforating collagenosis, acquired perforating dermatosis, perforating periumbilical calcific elastosis, and perforating granuloma annulare [1].
Approximately 40 percent of patients with EPS have an underlying genetically-determined syndrome. Reported associations include trisomy 21, Ehlers-Danlos syndrome, osteogenesis imperfecta, Marfan disease, pseudoxanthoma elasticum, Rothmund-Thompson syndrome and acrogeria. In addition to these presumably genetically determined cases, a second subset of patients have acquired disorders such as diabetes mellitus, morphea and renal failure; a third subset develops EPS after therapy with penicillamine for Wilson disease, cystinuria, or rheumatoid arthritis [2].
Elastosis perforans serpiginosa most commonly manifests on the face, neck, and upper extremities [2]. The trunk or lower extremities may also be involved and EPS of the penis has been reported [2, 3]. The typical clinical manifestation consists of asymptomatic to pruritic grouped keratotic papules tending towards serpiginous or annular configurations. The lesions are indolent and may be stable for years [1].
Histologically, EPS demonstrates a hypertrophic epidermis with focal parakeratotic plugging. Beneath the area of plugging, there is a canal-like structure extending into the papillary dermis. Basophilic nuclear debris and eosinophilic elastic fibers are observed within this channel. Elastic tissue stains highlight these fibers, though usually more weakly than normal elastic fibers. Additionally, occasional foreign body giant cells as well as acute inflammatory cells may be observed [4, 5].
Treatment of EPS is difficult and most methods are reported to have limited success. Reported ablative treatments include cellophane tape stripping, electrodesiccation, and curettage, cryotherapy, glycolic acid, salicylic acid, flashlamp pulsed-dye, erbium:yttrium-aluminum-garnet, and carbon dioxide laser [5, 6, 7, 8]. Other reported modalities include oral and topical retinoids [9, 10], intralesional and topical steroids [10], topical calcipotriene [7], and narrow band ultraviolet B radiation [7].
References
1. Jean L. Bolognia, Ronald P. Rapini, ed. Dermatology. 1 ed. 2003, Elsevier Science: Philadelphia. 2460.2. Lewis KG, Bercovitch L, Dill SW, Robinson-Bostom L. Acquired disorders of elastic tissue: part I. Increased elastic tissue and solar elastotic syndromes. J Am Acad Dermatol. 2004 Jul;51(1):1-21; quiz 22-4. PubMed
3. Roest MA, Ratnavel R. Elastosis perforans serpiginosa of the penis. BJU Int, 2003 Mar;91(4):427. No abstract available. PubMed
4. Weedon D. Skin Pathology. 2 ed. 2002, Philadelphia: Elsevier Science. 1158.
5. Saxena M, Tope WD. Response of elastosis perforans serpiginosa to pulsed CO2, Er:YAG, and dye lasers. Dermatol Surg. 2003Jun;29(6):677-8. No abstract available. PubMed
6. Tuyp EJ, McLeod WA. Elastosis perforans serpiginosa: treatment with liquid nitrogen. Int J Dermatol. 1990 Nov;29(9):655-6. No abstract available. PubMed
7. Mehta RK, Burrows NP, Payne CM, Mendelsohn SS, Pope FM, Rytina E. Elastosis perforans serpiginosa and associated disorders. Clin Exp Dermatol. 2001 Sep;26(6):521-4. PubMed
8. Kaufman AJ. Treatment of elastosis perforans serpiginosa with the flashlamp pulsed dye laser. Dermatol Surg. 2000 Nov;26(11):1060-2. PubMed
9. Ratnavel RC, Norris PG. Penicillamine-induced elastosis perforans serpiginosa treated successfully with isotretinoin. Dermatology. 1994;189(1):81-3. PubMed
10. Outland JD, Brown TS, Callen JP. Tazarotene is an effective therapy for elastosis perforans serpiginosa. Arch Dermatol. 2002 Feb;138(2):169-71. PubMed
© 2006 Dermatology Online Journal