Streptococcal toxic shock syndrome and sepsis manifesting in a patient with chronic rheumatoid arthritis
Published Web Location
https://doi.org/10.5070/D31cv3g69zMain Content
Streptococcal toxic shock syndrome and sepsis manifesting in a patient with chronic rheumatoid arthritis
Shylashree Chikkamuniyappa
Dermatology Online Journal 10 (1): 7
Department of Pathology, University of Texas Health Science Center at San Antonio. chikkamuniya@uthscsa.edu
Abstract
Streptococcal-toxic-shock syndrome is caused by virulent strains of exotoxin-producing streptococcus, almost always group-A organisms such as Streptococcus pyogenes. It has often been described in the setting of surgical wounds, burns, childbirth, diabetics, elderly, neonates, and immunocompromised hosts, where the portal of entry is the skin. Our patient was on steroids and nonsteroidal anti-inflammatory drugs for chronic rheumatoid arthritis and developed this deadly infection after a fall.
Streptococcal-toxic-shock syndrome is caused by virulent strains of exotoxin-producing streptococcus, almost always group-A organisms such as Streptococcus pyogenes [1]. It has often been described in the setting of surgical wounds, burns, childbirth, diabetics, elderly, neonates, and immunocompromised hosts, where the portal of entry is the skin. Our patient was on steroids and nonsteroidal anti-inflammatory drugs for chronic rheumatoid arthritis and developed this deadly infection after a fall.
Rapidly progressive soft-tissue infections generally constitute either a cellulitis or a necrotizing process, including necrotizing fasciitis from an infectious organism. Necrotizing fasciitis commences as a poorly defined area of erythema progressing to serosanguinous blisters and then subsequent necrosis at the center [2]. Constitutional symptoms are present and there is a significant mortality.
Clinical summary
A 68-year-old man was admitted to the emergency room in the middle of the night with pain and swelling of his right upper extremity. He had multiple hemorrhagic blisters and bullae with advancing erythema on the right upper extremity, right chest, and abdomen. He reported a fall on the elbow 3-days prior, with development of a small erythematous macule on the right forearm; the macule gradually progressed to multiple hemorrhagic fragile bullae involving the entire right extremity and extending to the chest and abdomen.
The patient also has a history of chronic rheumatoid arthritis and was on steroids, hydroxychloroquine and leflunomide. There was no recent travel or use of illicit drugs; he had no recent exposure to ill persons and no known insect bites.
|
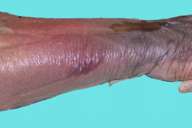
| Figure 1 |
|---|
| Right forearm |
The patient was febrile, tachycardic, tachypneic, and had nausea with vomiting. The upper extremity was swollen with superficial necrosis and numerous areas of skin breakdown. The patient appeared ill, pale, and was in extreme pain. The pulses were intact. He developed severe hypotension, acute renal failure, metabolic acidosis, respiratory alkalosis, and septic shock. Significant laboratory findings include a white blood count of 14.39 cells/mm³ (86 % neutrophils), BUN of 31mg/dl, creatinine of 2.7 mg /dl, and fractional excretion of sodium < 1.
The differential diagnosis included compartment syndrome, cellulitis, scalded skin syndrome, toxic epidermal necrolysis, and necrotizing fasciitis. A punch biopsy of the skin was non-contributory. Blood cultures showed Group-A β-hemolytic streptococci (Streptococci pyogenes). The patient was treated with intravenous antibiotics (1g Vancomycin, 2.25g Zosyn, 2 million units Penicillin G and 600mg Clindamycin). After intubation and sedation, he underwent a right upper extremity and forequarter amputation with excision of the skin and soft tissue of the right anterior chest wall and abdomen. This procedure involved removing 35 percent of his body surface area, his right scapula, and two thirds of right clavicle with the right pectoralis major and minor, latissimus dorsi, serratus anterior, deltoid, rotator cuff muscle and rhomboids. Incision of the indurated areas showed considerable fluid but, no purulence, involving subcutaneous fat. Muscle tissue beneath the fascia was pink to necrotic. The wound was debrided and irrigated with large volumes of normal saline and an antibiotic solution. A drain was inserted, and the incision was not closed.
|
|
| Figure 2 | Figure 3 |
|---|---|
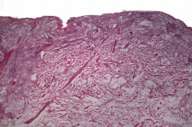
| Low power view of severe epidermal and dermal necrosis (Fig. 2) (10X, H&E) | |
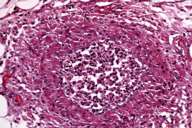
| Vasculitis (fig. 3)(40X, H&E) | |
Histopathology showed severe necrosis involving the epidermis, dermis, and subcutis (fig. 2). There was vasculitis, sometime associated with occlusion of the lumen by thrombi. There was a mixed inflammatory cell infiltrate with numerous neutrophils (Fig. 3).
|
|
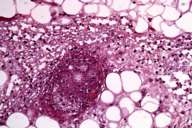
| Figure 4 | Figure 5 |
|---|---|
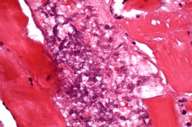
| Myositis with numerous bacterial colonies (Fig. 4) and associated fat necrosis (fig. 5) (40X, H&E). | |
Currently the patient is doing well and is expected to make a complete recovery and on his way to multiple graft revisions.
Discussion
Cellulitis involves the dermis and subcutaneous fat. It can result from penetration of the skin, extension from a contiguous focus, or hematogenous seeding from a distant focus (especially in an area of blunt trauma or other injury). Group-A streptococci and S. aureus are the most common causal organisms of cellulitis. Cellulitis can progress to necrotizing fasciitis and toxic shock syndrome owing to the production of exotoxins.
Necrotizing fasciitis involves fascial necrosis with thrombosis of the subcutaneous blood vessels leading to cutaneous gangrene. Various organisms such as Pseudomonas, aeromonas, S. aureus, Streptococcus pneumoniae, Serratia, and Vibrio have been implicated.
Our case represents a necrotizing fasciitis with septic shock associated with group A β-hemolytic Streptococcal infection. This type of fasciitis is occasionally seen in conjunction with S. aureus. Streptococcal necrotizing fasciitis is a rapidly-progressive process and is associated with the toxic shock syndrome in up to 50 percent of cases; it has a mortality rate of 30-70 percent [3]. Streptococcal serotypes M1 and M3 most commonly produce pyogenic exotoxins that elicit a cascade of cytokine responses resulting in damage to multiple organ systems. Renal and hepatic compromise as well as pulmonary infiltrates and the development of the acute respiratory distress syndrome are common [4]. These organisms produce multiple enzymes, including hyaluronidase, which allows rapid spreading along fascial planes, and streptolysin and proteinase, which cause liquefaction of exudates. Streptococci may also produce pyogenic exotoxins, toxic superantigens that result in production of various cytokines, interleukins, and activation of macrophages.
The criteria for a diagnosis of streptococcal toxic shock syndrome include the isolation of group A streptococci, hypotension, and two or more of the following signs: coagulopathy; soft-tissue necrosis, including fasciitis, myositis, or gangrene; hepatic involvement; renal impairment; a generalized, erythematous, macular rash; and acute respiratory distress syndrome [5].
References
1. Stanford DG, Georgouras KE, Sullivan EA, Greenoak GE. Toxic streptococcal syndrome. Australas J Dermatol. 1997 Aug; 38(3): 158-60. PubMed2. Koehn GG. Necrotizing fascilitis. Arch Dermatol. 1979 Apr; 115(4): 507. PubMed
3. Kaul R, McGeer A, Low DE, Green K, Schwartz B. Population-based surveillance for group A streptococcal necrotizing fasciitis: Clinical features, prognostic indicators, and microbiologic analysis of seventy-seven cases. Ontario Group A Streptococcal Study. Am J Med. 1997 Jul; 103(1): 18-24. PubMed
4. Defining the group A streptococcal toxic shock syndrome. Rationale and consensus definition. The Working Group on Severe Streptococcal Infections. JAMA. 1993 Jan 20; 269(3): 390-1. PubMed
5. Bisno AL. Streptococcus pyogenes. In: Mandell GL, Bennett JE, Dolin R, eds. Mandell, Douglas and Bennett's principles and practice of infectious diseases. 4th ed. Vol. 2. New York: Churchill Livingstone, 1786-1799,1995
© 2004 Dermatology Online Journal

